
Title: Depression Disorders in the DSM 5 TR Symptoms and Diagnosis
Channel: Doc Snipes
Depression Disorders in the DSM 5 TR Symptoms and Diagnosis by Doc Snipes
bipolar depression dsm 5 diagnosis, bipolar 2 disorder dsm 5 definition, dsm 5 diagnostic code for bipolar disorder, dsm-5 diagnostic criteria for bipolar disorder, dsm-5 bipolar disorder symptoms, dsm criteria for bipolar depression
Bipolar Depression: DSM-5 Diagnosis—Is THIS the Missing Piece of Your Puzzle?
Unraveling the Shadows: Decoding Bipolar Depression and the DSM-5
It's time we shed some light on bipolar depression. It's a complex condition. It can feel like an unsolvable puzzle. The DSM-5 offers clues. It's the diagnostic manual. This manual tries to help. It can help clarify things. Are you feeling lost? This might be the piece you seek.
A Landscape of Shifting Moods: Understanding the Essence
Bipolar depression isn't simple sadness. It goes beyond fleeting blues. It's a rollercoaster of emotions. There are extreme highs, then plummeting lows. Sometimes, these shifts happen quickly. Consequently, it’s tough to cope. The impact can be profound. It affects your life drastically. Therefore, let's explore these shifts.
The DSM-5: Your Diagnostic Compass
The DSM-5 is crucial. It provides diagnostic criteria. It's a guide for mental health professionals. Professionals use it to understand your symptoms. Several key markers diagnose bipolar depression. These indicators help confirm the diagnosis. However, it's not always straightforward.
Diving Deep: Key Symptoms to Recognize
Recognizing symptoms is the first step. Persistent sadness is common. Loss of interest is another sign. Changes in sleep patterns also occur. Appetite fluctuations often appear, too. Feeling fatigued often accompanies it. Difficulty concentrating is another symptom. Thoughts of suicide can, unfortunately, arise. If these persist, seek help immediately. Furthermore, mania or hypomania episodes exist.
The Diagnostic Dance: Unpacking the Criteria
The diagnostic process involves several steps. Assessment by a mental health professional is essential. They'll ask about your history. They'll also ask about your symptoms. The DSM-5 criteria are then applied. Bipolar I includes manic episodes. Bipolar II involves hypomania and depression. Your specific pattern is important.
Unmasking the Misconceptions: Dispelling Common Myths
There are many myths about bipolar disorder. It's definitely not a character flaw. It's a real medical condition. It requires professional treatment. Medication and therapy can help. Support systems are vital as well. Let's dispel some common misunderstandings.
Navigating the Nuances: Differentiating From Other Conditions
Depression can mask bipolar disorder. Symptoms can overlap with other illnesses. Proper diagnosis is crucial. A thorough evaluation is necessary. Differentiating is vitally important. Therefore, experts must carefully assess the situation. They rule out other possibilities. This is key to effective treatment.
Crafting Your Personalized Path to Wellness: Treatment Strategies
There are effective treatment paths. Medication often plays a significant role. Antidepressants alone can sometimes be counterproductive. Mood stabilizers are often included. Psychotherapy provides support. Cognitive behavioral therapy (CBT) can help. Lifestyle adjustments also matter. Regular exercise is beneficial. Healthy sleep habits help too. A good support system reduces isolation.
Empowering Your Journey: A Guide to Self-Care
You can take proactive steps, always. Educate yourself about bipolar disorder. Learn your triggers and warning signs. Develop coping skills and strategies. Build a support network of trusted people. Prioritize self-care daily. Practice mindfulness and relaxation techniques. Celebrate your successes.
Finding the Missing Piece: The Importance of Advocacy
Advocacy helps everyone involved. Support research and mental health awareness. Share your story if you feel comfortable. Raise awareness within your circle. Fight the stigma. By helping others, you also help yourself.
The Path Ahead: Maintaining Balance and Hope
Living with bipolar depression isn't easy. It's a lifelong journey. There are ups and downs. However, it's possible to thrive. With the right treatment and support, you can manage your symptoms. You can live a fulfilling life. Remember the importance of hope. Never give up on yourself. Therefore, prioritize yourself. Then, pursue wellness.
Banish Your Blues: Bible Verses That Will Actually Lift Your DepressionBipolar Depression: DSM-5 Diagnosis—Is THIS the Missing Piece of Your Puzzle?
Okay, let's be real for a second. Navigating the world of mental health can feel like trying to solve a Rubik's Cube blindfolded, underwater, during an earthquake. It's complex, confusing, and often, downright frustrating. And when we’re talking about something as nuanced as bipolar depression, the waters get even murkier. So, grab a cup of coffee (or tea, or whatever fuels your engine!), and let's dive in. We're going to break down the DSM-5 diagnosis of bipolar depression and explore whether it holds the key to finally unlocking, or at least understanding, your own personal puzzle.
1. The Rollercoaster Ride: Understanding Bipolar Disorder
Think of bipolar disorder as a rollercoaster. Sometimes you’re soaring high, feeling invincible and bursting with energy (mania/hypomania), and other times, you’re plummeting into the depths of despair and hopelessness (depression). It’s a mood disorder, and it’s characterized by these extreme shifts. But it's not just feeling sad or happy. It's experiencing moods that are significantly different than what's considered normal for you, and that severely impacts your day-to-day functioning.
2. The Diagnostic and Statistical Manual of Mental Disorders (DSM-5): Your Guide to the Maze
The DSM-5 is the "bible" of mental health diagnoses. It's a comprehensive guide containing the criteria that mental health professionals use to diagnose various conditions, including bipolar disorder. It’s like a meticulously detailed map leading us through the complex terrain of our minds. This isn't something you can self-diagnose with, but understanding its framework can be incredibly empowering as you navigate conversations with your mental health team.
3. Unpacking Bipolar Depression: More Than Just the Blues
Depressive episodes in bipolar disorder are different from major depressive disorder. The key distinction, and a crucial piece of the puzzle, is the presence (or history) of manic or hypomanic episodes. While they may seem similar, the underlying causes and treatment approaches often differ significantly. We're not just talking about feeling sad; it's a deep despair that can feel all-consuming.
4. Mania vs. Hypomania: What's the Difference?
Here's where things get nuanced. Mania is the more intense of the two, a full-blown episode that can include everything from reckless behavior and racing thoughts to severe irritability and even psychosis. Hypomania is a milder form of mania. It still involves elevated mood and energy, but it’s generally less disruptive. Think of it as a souped-up version of your normal self.
- Mania: Extreme, often leading to hospitalization, significant impairment.
- Hypomania: Noticeable, but may not require hospitalization, less significant impairment.
5. The DSM-5 Criteria for Bipolar I Disorder (The Big Boys)
For a diagnosis of Bipolar I Disorder, the DSM-5 requires at least one manic episode. This manic episode has to be severe enough to cause significant impairment in your daily life or require hospitalization. Depressive episodes are also often present, but the defining characteristic is that manic episode. This is a crucial piece of the puzzle when clinicians are determining a diagnosis.
6. The DSM-5 Criteria for Bipolar II Disorder (The Hypomanic Side)
Bipolar II Disorder involves at least one hypomanic episode and a major depressive episode. The key distinction from Bipolar I is the absence of full-blown manic episodes. It's important to remember that the depressive episodes in Bipolar II can be just as debilitating as those in Bipolar I, even without the manic highs. This is something many people miss and it's a key element to understanding this complex disorder.
7. Cycling Through the Seasons: Recognizing the Patterns
The symptoms of bipolar depression can vary. Some people might cycle quickly between moods (rapid cycling), while others might experience longer periods of depression or mania. Recognizing your personal patterns is critical. Journaling, tracking your mood, and working closely with your clinician can help you identify those patterns and potentially predict them.
8. Beyond the Blues: The Symptoms to Watch For
Depressive symptoms in bipolar disorder can look like any other major depressive episode, but there are subtle differences. They can include:
- Persistent sadness, hopelessness, or emptiness
- Loss of interest in activities you used to enjoy
- Changes in appetite or weight
- Sleep disturbances (insomnia or sleeping too much)
- Fatigue or loss of energy
- Feelings of worthlessness or guilt
- Difficulty concentrating or making decisions
- Thoughts of death or suicide (this always requires immediate attention)
9. The Diagnostic Process: What to Expect
Getting a diagnosis can feel like a long journey, and frankly, it is. It involves a thorough evaluation by a qualified mental health professional—usually a psychiatrist or a psychologist. This includes a detailed interview about your symptoms, medical history, family history, and any prior experiences of mental health treatment. They might also use questionnaires and rating scales to assess your mood and functioning.
10. Filling in the Gaps: Why Accurate Diagnosis Matters
Accurate diagnosis is paramount because it informs the treatment plan. Without knowing the type of bipolar disorder, and even understanding the details of your experience, you can't get the right treatment. What works for major depressive disorder might not work, or even make, bipolar depression better.
11. Treatment Strategies: Finding Your Footing
Treatment for bipolar depression typically involves a combination of medication and therapy. Mood stabilizers are often the cornerstone of treatment. Antidepressants can be used to help manage the depressive symptoms, but they must be carefully managed to avoid triggering a manic episode. Therapy, such as cognitive behavioral therapy (CBT) or interpersonal and social rhythm therapy (IPSRT), can help you manage your moods, develop coping strategies, and improve your overall well-being.
12. The Power of Support: Building Your Team
Dealing with bipolar depression is a team sport. You need a supportive network of friends, family, and mental health professionals. Never underestimate the power of talking to someone who understands what you're going through. Support groups, online communities, and individual therapy can all provide invaluable support.
13. Living Well with Bipolar Depression: Tips for Thriving
Living well with bipolar depression is possible. It’s about embracing self-care, establishing healthy routines, and learning to manage your moods. This includes getting enough sleep, eating a balanced diet, exercising regularly, avoiding alcohol and drugs (which can worsen symptoms), and taking your medications as prescribed.
14. The Missing Piece: Is This the Key to Your Own Puzzle?
Perhaps. Understanding the DSM-5 diagnostic criteria is a powerful first step. It can help you better understand what you're going through, advocate for yourself, and work with your mental health team to find the right path forward. It helps to see your experience through an educated lens.
15. Seeking Professional Help: When to Take Action
If you're experiencing symptoms of depression, or suspect you have bipolar disorder, don't hesitate to reach out for professional help. It’s often the hardest step, but trust me: it's the most worthwhile. Find a mental health professional you trust, and be honest and open about your experiences. Your mental health matters.
Closing Thoughts
So, there you have it. A deep dive into the DSM-5 diagnosis of bipolar depression. Remember, this is a complex condition, and there's no one-size-fits-all answer. But by understanding the criteria, recognizing the symptoms, and seeking the appropriate treatment, you can take control of your life and find your way to a happier, healthier you. You are not alone; help is always available.
FAQs
1. Can bipolar depression be cured?
Bipolar disorder typically isn't "cured" in the traditional sense, but it can be effectively managed. With the right treatment, including medication and therapy, many people with bipolar disorder live fulfilling and productive lives. Think of it like managing diabetes: You can't "cure" it, but you can absolutely control it and live a full life.
2. What if I'm misdiagnosed?
Misdiagnosis is a real possibility, especially in the early stages. If you feel your diagnosis doesn't fit, or if your treatment isn't working, don't hesitate to seek a second opinion. It is your right. Thoroughly evaluate your symptoms with a skilled specialist.
3. What if I think I'm experiencing hypomania?
Hypomania is a tricky beast. It can feel good, like you have super-powers. If you suspect you're experiencing hypomania, talk to your doctor immediately. They may adjust your medication or therapy or adjust your therapy to fit your needs.
4. Is bipolar disorder genetic?
Yes, genetics play a significant role, with a family history increasing your risk. However, it's not a guarantee. Environmental factors and life experiences also contribute to the development of the disorder.
5. Where can I find support?
There are countless resources available! Start with your primary care physician, who can recommend a mental health professional. Search online support groups, or consult with organizations like the Depression and Bipolar Support Alliance (DBSA) or the National Alliance on Mental Illness (NAMI). It's important to find a community that supports you.
Is Your Child Secretly Depressed? Shocking New Guidelines Revealed!Bipolar Disorder Assessment and Diagnosis Living with Bipolar Disorder

By Doc Snipes Bipolar Disorder Assessment and Diagnosis Living with Bipolar Disorder by Doc Snipes
Bipolar Disorder Type 1 vs Type 2 Risk Factors, Symptoms, Diagnosis, Treatment

By JJ Medicine Bipolar Disorder Type 1 vs Type 2 Risk Factors, Symptoms, Diagnosis, Treatment by JJ Medicine
Bipolar Disorder Symptoms, Risk Factors, Causes, Diagnosis and Treatments, Animation
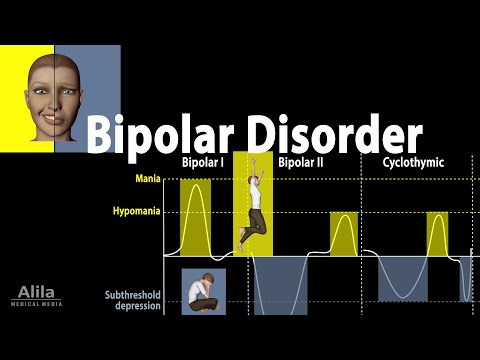
By Alila Medical Media Bipolar Disorder Symptoms, Risk Factors, Causes, Diagnosis and Treatments, Animation by Alila Medical Media

Title: Bipolar and related disorders - causes, symptoms, treatment & pathology Updated 2024
Channel: Osmosis from Elsevier
Bipolar and related disorders - causes, symptoms, treatment & pathology Updated 2024 by Osmosis from Elsevier
Depression Glass Ballerina: The Pattern You NEED to See!
Bipolar Depression: DSM-5 Diagnosis—Is THIS the Missing Piece of Your Puzzle?
We understand. You're here because something feels profoundly amiss. Perhaps you’ve been living a life punctuated by periods of soaring highs and crushing lows. Or, maybe you’re navigating a persistent undercurrent of despair, a relentless fog that obscures any glimmer of joy. You suspect something deeper is at play, a hidden force shaping your emotional landscape. If these thoughts resonate, you might be contemplating a diagnosis of bipolar depression, and if you're here, you're likely seeking answers. We're here to help you clarify one of the most critical aspects of your journey: the diagnostic process.
This article will delve into the DSM-5 criteria for diagnosing bipolar depression, providing a clear, concise exploration of the diagnostic framework. We’ll explore the specific symptoms, the nuances that separate it from unipolar depression, and what it truly means for those experiencing it. We'll work with you as you journey through the pieces that will make you whole.
Unraveling the Diagnostic Criteria: The DSM-5 Blueprint
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), published by the American Psychiatric Association, serves as the definitive guide for mental health professionals. It provides standardized criteria for diagnosing mental health conditions, including bipolar disorders. Understanding the DSM-5 criteria is vital for anyone seeking a diagnosis, as it provides the framework doctors and therapists will use to assess your condition accurately.
For a diagnosis of bipolar depression, the diagnostic process starts with the recognition of a major depressive episode. This is the foundation, the anchoring point from which the rest of the diagnostic criteria radiate. To meet the criteria for a major depressive episode, you must experience at least five of the following symptoms during the same two-week period, and at least one of the symptoms must be either depressed mood or loss of interest or pleasure:
- Depressed Mood: This is a persistent feeling of sadness, emptiness, or hopelessness. It's not simply a passing bad day; it’s a pervasive emotional state that colors your perception of the world.
- Loss of Interest or Pleasure (Anhedonia): Activities that once brought joy now feel flat, meaningless, or apathetic. The spark is gone. Hobbies, social interactions, even basic pleasures like eating or listening to music can lose their appeal.
- Significant Weight Loss or Gain: A noticeable change in weight when not dieting, or a decrease or increase in appetite nearly every day.
- Insomnia or Hypersomnia: Trouble sleeping, or sleeping practically all day, nearly every day.
- Psychomotor Agitation or Retardation: Feeling restless and agitated, pacing around the room, or feeling slowed down and sluggish.
- Fatigue or Loss of Energy: Feeling tired or depleted, experiencing a constant sense of weariness, making it difficult to accomplish daily tasks.
- Feelings of Worthlessness or Excessive Guilt: Intense feelings of self-doubt, worthlessness, or inappropriate guilt that may or may not be delusional.
- Difficulty Concentrating or Making Decisions: Trouble focusing, remembering things, or making even simple choices.
- Recurrent Thoughts of Death or Suicidal Ideation: Thinking about death, suicidal ideation, or a suicide attempt, with or without a specific plan.
Distinguishing Bipolar Depression: The Crucial "History" Element
However, meeting the criteria for a major depressive episode alone doesn't automatically equate to a diagnosis of bipolar depression. This is where the critical distinction arises. In bipolar disorder, the defining characteristic lies in the history of episodes of mania or hypomania. This is the key differentiating factor, the crucial piece that completes the puzzle.
- Mania: A distinct period of abnormally and persistently elevated, expansive, or irritable mood and abnormally and persistently increased activity or energy, lasting at least one week and present most of the day, nearly every day. During the period of mood disturbance and increased energy or activity, at least three of the following symptoms are present (four if the mood is only irritable):
- Inflated self-esteem or grandiosity.
- Decreased need for sleep (e.g., feels rested after only 3 hours of sleep).
- More talkative than usual or pressure to keep talking.
- Flight of ideas or subjective experience that thoughts are racing.
- Distractibility (i.e., attention too easily drawn to unimportant or irrelevant external stimuli), as reported or observed.
- Increase in goal-directed activity (either socially, at work or school, or sexually) or psychomotor agitation.
- Excessive involvement in activities that have a high potential for painful consequences (e.g., engaging in unrestrained buying sprees, sexual indiscretions, or foolish business investments).
- Hypomania: A distinct period of persistently elevated, expansive, or irritable mood and persistently increased activity or energy, lasting at least four days and present most of the day, nearly every day. The episode is associated with a definite change in functioning that is uncharacteristic of the individual when not symptomatic. The episode is observable by others. The episode is not severe enough to cause marked impairment in social or occupational functioning or to necessitate hospitalization. If psychotic features are present, the episode, by definition, is a manic episode.
The diagnosis of bipolar depression hinges on whether a person has experienced at least one episode of mania or hypomania in their lifetime. This is why a thorough psychiatric evaluation, including a detailed history of your moods, is crucial. The doctor will meticulously examine your past experiences, looking for evidence of elevated moods, increased energy, impulsivity, and any other symptoms indicative of mania or hypomania.
Navigating the Diagnostic Process: Your Role and What to Expect
The diagnostic process is a collaborative journey between you and a qualified mental health professional, typically a psychiatrist or a clinical psychologist. Here’s what you can expect:
- Comprehensive Interview: The mental health professional will conduct a detailed interview, delving into your medical history, family history of mental illness, and current symptoms. They will ask specific questions about your mood fluctuations, sleep patterns, energy levels, and behavior.
- Symptom Assessment: The professional will carefully assess your current symptoms, looking for the specific criteria listed in the DSM-5. They will use standardized questionnaires and rating scales to quantify your symptoms and track their severity.
- Mood Charting: Keeping a mood chart can be immensely helpful. This involves tracking your daily moods, energy levels, sleep patterns, and any other relevant symptoms. This provides valuable information and will help identify patterns and cycles.
- Gather Information: You may be asked to provide collateral information, such as from a family member or close friend, to gain a broader perspective on your behavior and history. This information is often critical for assessing the presence of mania or hypomania.
- Differential Diagnosis: The mental health professional will consider other potential diagnoses, such as major depressive disorder, anxiety disorders, or other conditions, to ensure accurate diagnosis. They will eliminate other possibilities to arrive at an accurate diagnosis.
- Treatment Plan: If a diagnosis of bipolar depression is made, the mental health professional will develop a comprehensive treatment plan, which may involve medications, therapy, or a combination of both.
Understanding the Implications: The Path Forward
Receiving a diagnosis of bipolar depression is a significant step, but it's also a gateway to effective treatment and a better quality of life. It provides a framework for understanding your experiences and allows you to access the necessary care.
Here's what this means for you:
- Accurate Diagnosis: The diagnosis helps you, your support system, and your treatment team understand the underlying cause of your symptoms. This is the foundation for effective treatment.
- Targeted Treatment: Treatment options are tailored specifically to bipolar depression, including mood-stabilizing medications, psychotherapy, and lifestyle adjustments. You can work with your mental health professional to find the right combination that is best for you.
- Symptom Management: Treatment aims to stabilize your mood, reduce the frequency and intensity of episodes, and improve your overall quality of life. You can regain control, stability, and satisfaction in everyday life.
- Empowerment: With the correct tools and guidance, you can learn to manage your condition, identify triggers, and build resilience.
- Improved Well-being: Bipolar depression can be managed with appropriate care, enabling you to live a fulfilling and productive life.
Conclusion: Taking the First Step
The diagnostic process for bipolar depression can feel overwhelming, but it's a necessary step toward healing. Understanding the DSM-5 criteria, working closely with a qualified mental health professional, and actively participating in your care are essential elements of your journey. Once you begin the process, it will not be long before you have found what you need. Do not worry. You can achieve a more stable and joyful life.
