
Title: Bipolar disorder depression & mania - causes, symptoms, treatment & pathology
Channel: Osmosis from Elsevier
Bipolar disorder depression & mania - causes, symptoms, treatment & pathology by Osmosis from Elsevier
manic depression icd 10, mania depression icd 10, bipolar manic depression icd 10, manic depression hcc icd 10, manic depressive episode icd 10, bipolar disorder manic depression icd 10, bipolar depression unspecified icd 10, bipolar 2 depression icd 10, bipolar depression severe icd 10
Manic Depression (ICD-10): The Shocking Truth Doctors Don't Want You to Know
Unmasking the Shadows: Untangling the Complexities of Bipolar Disorder
The world of mental health often feels veiled. Specifically, bipolar disorder carries a heavy weight. Moreover, it's a multifaceted condition, therefore understanding it is crucial. This article aims to shed light on this often misunderstood illness. It bypasses the sensationalism. Instead, it focuses on clear, accessible information.
The Dance of Extremes: A Look at the Bipolar Spectrum
Bipolar disorder isn't a simple diagnosis. It’s a spectrum, you see. This means it presents a wide range of experiences. At one end lie periods of intense mania. Conversely, at the opposite end are the depths of depression. These phases can alternate, or even overlap. The severity varies drastically from person to person. Consequently, the impact on daily life is significant.
Think of it like a seesaw, constantly in motion. One moment, you're soaring high. The next, you're plummeting down. This unpredictable nature is a hallmark of the disorder. Consequently, the individual and their loved ones face unique challenges.
Beyond the Label: Recognizing the Subtle Signs
Detecting bipolar disorder can be tricky. The symptoms are often misinterpreted. Furthermore, the condition mimics other illnesses. Mania doesn't always look like reckless behavior. It can manifest as irritability, restlessness, even racing thoughts. On the flip side, depression might appear like prolonged sadness. It can also include changes in sleep, appetite, or energy levels.
Therefore, paying close attention to patterns is key. Mood swings are normal, yet frequent or extreme shifts warrant attention. Additionally, family history plays a role. Genetic predisposition increases the likelihood. Early intervention improves outcomes significantly.
The Impact on Relationships: Navigating the Storm
Bipolar disorder dramatically affects relationships. The fluctuations in mood create strains. Manic episodes can lead to impulsive decisions. These decisions may involve financial recklessness or inappropriate behavior. Depressive phases, then, can cause withdrawal and isolation.
Furthermore, maintaining open communication is crucial. Mutual understanding empowers everyone involved. Educating friends and family helps. It also fosters empathy and support. It’s a collaborative effort. Remember, you're not alone.
Seeking Support: A Path Towards Stability
Living well with bipolar disorder is achievable. Treatment is often multi-faceted. Medication frequently plays a central role. Mood stabilizers and antidepressants can help regulate moods. Therapy is equally vital. Cognitive Behavioral Therapy (CBT) teaches coping strategies. Interpersonal therapy addresses relationship difficulties.
Therefore, never hesitate to seek professional help. Mental health specialists are experts in this field. Creating a strong support system is essential. This could include support groups. It also includes trusted friends and family. Self-care is critical. Consistent sleep, healthy eating, and regular exercise contribute to stability.
The Ongoing Journey: Embracing Growth and Resilience
Living with bipolar disorder is a lifelong journey. There will be ups and downs, without a doubt. However, setbacks don't define a person. They provide opportunities for growth. Learning to manage symptoms is key. Practicing self-compassion is also fundamental.
Moreover, celebrate successes. Acknowledge your resilience. Focus on the present moment. Remember your value. Embrace your unique strengths. Bipolar disorder can be managed effectively. Living a fulfilling life is possible. Take things one day at a time. Keep learning. Keep growing. Find your path to wellness. The journey is worth it.
Is Your Baking Depressed? (Shocking Truth Inside!)Manic Depression (ICD-10): The Shocking Truth Doctors Don't Want You to Know
Hey everyone, let's talk about something that affects millions, yet is often misunderstood and shrouded in secrecy: Manic Depression, officially known as Bipolar Disorder, and diagnosed using the ICD-10 classification system. It can feel like a rollercoaster you didn't sign up for, one that's often downplayed or even completely missed by those who should be helping. We're going to peel back the layers and dig into the stuff doctors might not tell you – the nitty-gritty, the painful realities, and, hopefully, the path towards understanding and managing this challenging condition. Trust me, you're not alone, and it's okay to feel overwhelmed. Let's get started! This isn't meant to be a medical manual, but a conversation, a sharing of experiences, and a glimpse into the often-hidden world of Bipolar Disorder.
1. What Is This Beast Called Manic Depression?
Let's start with the basics. Manic Depression, or Bipolar Disorder, is a serious mental illness marked by extreme shifts in mood, energy, and activity levels. Imagine the highest highs and the lowest lows imaginable. You're soaring one moment, full of boundless energy and grand ideas, and the next you're plunged into a pit of despair, feeling hopeless and utterly exhausted. These mood swings aren't just "feeling a little down" or "being in a good mood." They're intense, disruptive, and can significantly impact your life, relationships, and work. ICD-10 provides a standardized way for doctors to diagnose and classify the different types of Bipolar Disorder, helping them tailor treatment plans.
2. The Two Sides of the Coin: Mania and Depression
Think of it like this: Bipolar Disorder has two primary faces: mania and depression. Mania is characterized by an elevated or irritable mood, inflated self-esteem (feeling like you can conquer the world!), decreased need for sleep (working 24/7!), racing thoughts, and risky behaviors (spending sprees, impulsive decisions). It's like being on a permanent high, but without the fun. Depression, on the other hand, is the crushing weight of sadness, hopelessness, loss of interest, fatigue, and sometimes thoughts of suicide. It's the feeling that you're drowning, and there's no way out.
3. The Hidden Truth: Misdiagnosis and Delayed Help
Here's where things get tricky. Often, the symptoms are shrugged off or misdiagnosed. We see this all the time. A person might only seek help when they're in a depressive episode, masking the manic phases that came before, leaving the doctors clueless. Doctors don't always have the time or training to spot the subtle clues that indicate Bipolar Disorder. Sometimes, it is wrongly diagnosed as simple depression. The delay in getting the right diagnosis and treatment can be devastating and cost valuable time.
4. Beyond the Basics: Types of Bipolar Disorder
There isn't a "one size fits all" approach. Bipolar Disorder is a spectrum. The ICD-10 helps distinguish between different types.
- Bipolar I Disorder: Characterized by manic episodes that last at least a week and may include depressive episodes, too.
- Bipolar II Disorder: Involves major depressive episodes and hypomanic episodes (less severe mania).
- Cyclothymic Disorder: A milder form with fluctuating moods, but not severe enough to meet the criteria for Bipolar I or II.
5. The Shocking Reality: The Stigma Surrounding Mental Illness
Let's be honest: mental illness still carries a stigma. People often feel ashamed or embarrassed to talk about it. This silence only perpetuates the problem. The stigma can keep people from seeking help, fearing judgment from family, friends, colleagues, or society in general. This stigma also affects access to resources, insurance coverage, and even employment opportunities.
6. The Root of the Problem: Genetics, Environment, and More…
What causes Manic Depression? The exact cause isn’t known, but it's likely a combination of factors. Genetics play a big role, meaning if you have a family history, your risk is higher. Environmental factors, such as stress, trauma, or substance abuse, can also trigger or worsen episodes. Often, it is a complex interplay, like a recipe where each ingredient plays a critical rule.
7. Unmasking the Triggers: What Sets Off the Rollercoaster?
Identifying your triggers is a crucial step in managing Bipolar Disorder. Triggers can vary from person to person but common examples include:
- Stress: Big life changes, relationship problems, or work pressure.
- Sleep Disruption: Lack of sleep or changes in sleep patterns.
- Substance Abuse: Alcohol, drug use.
- Medication Changes: Not taking medication as prescribed or stopping abruptly.
- Seasonal Changes: Some people have seasonal patterns to their mood shifts.
8. The Importance of Early Intervention & Treatment
Early diagnosis and treatment are critical. The longer someone goes untreated, the more severe the episodes can become, and the higher the risk of complications. A treatment plan typically involves medication, therapy, and lifestyle adjustments.
9. The Role of Medication: Finding the Right Balance
Medication is often a cornerstone of treatment. Mood stabilizers (like lithium), antidepressants, and antipsychotics are commonly prescribed. The goal is to regulate mood swings and provide greater stability. Finding the right medications and dosages can take time and require close communication with your psychiatrist.
10. Therapy Can Be Your Lifeline: Talking It Out
Therapy, such as Cognitive Behavioral Therapy (CBT) or Interpersonal and Social Rhythm Therapy (IPSRT), can provide valuable tools for managing symptoms, coping with challenges, and developing healthy coping mechanisms.
11. Lifestyle Matters: Small Changes, Big Impact
Taking care of your physical health is also crucial. Regular exercise, a healthy diet, a consistent sleep schedule, and avoiding alcohol and drugs can significantly improve your mood and stability. Imagine these lifestyle changes as your personal shield in the battle!
12. The Unspoken Truth: The Impact on Relationships
Bipolar Disorder can strain relationships, making it crucial to communicate openly with loved ones and educate them about the condition. Support groups for both the affected individual and their families can offer invaluable support and understanding.
13. Suicidal Thoughts: An Urgent Call for Help
Suicidal thoughts are a serious and potentially life-threatening symptom of Bipolar Disorder. If you or someone you know is experiencing suicidal thoughts, it is crucial to seek professional help immediately. Don't hesitate, and remember, you are not alone.
14. The Power of Support: Building Your Tribe
Having a strong support system is essential. Connect with friends, family, support groups, and mental health professionals. Build a community where you can feel safe, understood, and encouraged.
15. The Road to Recovery: It's a Marathon, Not a Sprint
Recovery is possible, but it's a journey, not a destination. There will be ups and downs. Be patient with yourself, celebrate your successes, and continue to seek support when you need it. With the right treatment, support, and self-care, you can live a fulfilling life!
In Conclusion: The journey with Manic Depression is far from easy. It's often a lonely path, marked by misunderstanding and stigma. But it doesn't have to be a life sentence. By understanding the truth, seeking help, and building a strong support system, we can overcome the challenges and live rich, meaningful lives. It's about taking control, finding the right resources, and fighting every day with confidence.
5 FAQs:
What are the early warning signs of a manic or depressive episode?
- Changes in sleep patterns, increased energy or fatigue, racing thoughts, irritability, changes in appetite, and withdrawal from social activities are all potential warning signs.
How do I talk to a loved one about their Manic Depression?
- Choose a calm time, focus on your concerns, and use "I" statements. Educate yourself about the condition to understand what they are going through. Encourage them to seek professional help.
What if medication doesn’t seem to be working perfectly?
- Talk to your doctor. Medication adjustment may be needed.
Can someone with Bipolar Disorder live a normal life?
- Yes! With treatment, therapy, and lifestyle management, most people with Bipolar Disorder can live fulfilling lives, maintain relationships, work, and realize their goals.
Where can I find support and resources?
- Start with your doctor or therapist. You can also research your local mental health services. If you're in crisis, dial your country's emergency number or go to your nearest hospital.
Principal Keywords: Manic Depression Truth Revealed
SEO Headline: Manic Depression Truth: Doctors Don't Tell You!
Pathway: /manic-truth/
Meta Summary: Shocking truths about Manic Depression (ICD-10) that doctors may not tell you. Unmask the stigma & find the path to knowledge & recovery. Your guide to understanding Manic Depression.
Bipolar Affective Disorder CAUSES, SYMPTOMS, ICD-10 CRITERIA & MANAGEMENT

By Medicine Made Simple Bipolar Affective Disorder CAUSES, SYMPTOMS, ICD-10 CRITERIA & MANAGEMENT by Medicine Made Simple
HOW TO REMEMBER THE CRITERIA FOR DEPRESSION ICD-10 CRITERIA MADE EASY

By Doctors' Infinite Potential HOW TO REMEMBER THE CRITERIA FOR DEPRESSION ICD-10 CRITERIA MADE EASY by Doctors' Infinite Potential
Bipolar Disorder Symptoms, Risk Factors, Causes, Diagnosis and Treatments, Animation
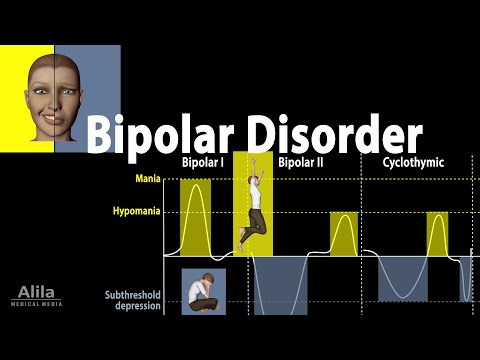
By Alila Medical Media Bipolar Disorder Symptoms, Risk Factors, Causes, Diagnosis and Treatments, Animation by Alila Medical Media

Title: Depression CAUSES, SYMPTOMS, ICD-10 CRITERIA & MANAGEMENT
Channel: Medicine Made Simple
Depression CAUSES, SYMPTOMS, ICD-10 CRITERIA & MANAGEMENT by Medicine Made Simple
Insomnia & Depression: The Shocking ICD-10 Code You NEED to Know
Manic Depression (ICD-10): The Shocking Truth Doctors Don't Want You to Know
We live in a world often painted with broad strokes, a world that simplifies complex realities. When it comes to mental health, this tendency towards simplification can be particularly dangerous. Manic depression, or what is clinically known as bipolar disorder, is frequently misunderstood and misrepresented. We are here to peel back the layers of this condition, to expose the nuanced truths, the lived experiences, and the crucial insights often sidelined in the usual narratives. This is not a surface-level exploration; this is a deep dive into the heart of a condition that affects millions, a condition we believe deserves a far more empathetic, and informed approach.
Unmasking the Fury: The Unpredictable Nature of Manic Episodes
The world rarely understands the full spectrum of a manic episode. It's often portrayed as an irrational high, a period of reckless spending, and impulsive decisions. While these behaviors can be present, they only scratch the surface of the internal chaos. A manic episode is a multifaceted experience involving altered perceptions of reality.
The hallmark is often a surging, relentless energy that feels both exhilarating and utterly consuming leading to a decreased need for sleep. A person in the throes of mania might go for days with little to no rest, yet feel vibrant and energetic. This insomnia isn't simply a lack of sleep; it's a break from the biological rhythm and can exacerbate the manic state. The individual's mind races. Thoughts cascade at lightning speed, making it challenging to focus on anything with the incessant mental chatter. This is not everyday hyperactivity; this is a torrent of ideas colliding and merging, often leading to grandiosity. They may develop inflated self-esteem. The individual can believe they possess special abilities, that they are on the verge of a great discovery, or that they are destined for something extraordinary. This overblown sense of self can lead to reckless decision-making; the purchase of expensive items, risky investments, and even dangerous behaviors.
It's important to realize that mania, at its core, is a distortion of reality. Perceptions are skewed. Judgment is impaired. Someone in a manic state may say or do things they'll later regret, sometimes with profound consequences. The emotional landscape is also unpredictable. While euphoria is a common feature, it's often intertwined with irritability, anger, and even paranoia. A simple frustration can escalate into an explosion of rage, which can damage their personal relationships. The intense highs are often followed by equally profound lows.
The Shadow of Depression: The Unseen Depths of the Cycle
The manic phase, however impactful, is merely one side of the coin. The depressive phase of bipolar disorder is often the predominant period and can be the most debilitating. This is where the true weight of the condition settles, a crushing burden of sadness, hopelessness, and despair.
Depression in bipolar disorder is not merely feeling "down." It's a pervasive state of overwhelming negativity. Motivation plummets, leaving the individual struggling to perform basic tasks. Everyday activities become monumental efforts. Getting out of bed, showering, or even eating can seem impossible, shrouded in a feeling of profound indifference.
Concentration struggles are severe, making it difficult to focus, read, or even hold a conversation. This cognitive impairment is often accompanied by feelings of worthlessness and guilt. A person may ruminate on past failures, or believe they are a burden to others. Suicidal ideation is a grave risk during these periods, which requires consistent attention and intervention from a qualified healthcare provider.
The physical symptoms compound the emotional pain. Fatigue is pervasive, and sleep disturbances are common. Appetite changes are experienced. These can lead to weight loss or gain. The body and mind become drained and exhausted. The individual will likely experience a significant loss of interest and pleasure in activities—a hallmark symptom of major depression.
The cycle is cruel, with the lows of depression often feeling inescapable. It's a constant battle against the darkness, a fight that requires the right support.
Beyond the Binary: The Different Faces of Bipolar Disorder
Many mistakenly view bipolar disorder as a uniform condition. The reality is more complex, with various subtypes, each bearing unique characteristics. Understanding these nuances is essential for proper diagnosis and effective treatment.
Bipolar I Disorder: This is the most commonly recognized form, characterized by the presence of at least one manic episode, which may be preceded or followed by a major depressive episode. The manic episodes are often severe, sometimes requiring hospitalization for safety reasons.
Bipolar II Disorder: This form involves recurrent episodes of major depression and hypomania, a less intense form of mania. While the hypomanic episodes might seem less disruptive than full-blown mania, they can still lead to impulsive behaviors. The depressive episodes are often the more prevalent and debilitating aspect of this subtype.
Cyclothymic Disorder: A chronic mood disorder characterized by fluctuating periods of hypomanic and depressive symptoms. These symptoms are less intense than those seen in bipolar I and II, but they persist for longer periods, creating an ongoing cycle of emotional upheaval.
Bipolar Disorder Not Otherwise Specified (NOS): This is a diagnostic category for individuals who do not fully meet the criteria for bipolar I, bipolar II, or cyclothymic disorder, but still exhibit symptoms consistent with the illness.
Recognizing these variations is key, as the treatment strategies must be tailored to the individual's specific symptoms and needs.
The Diagnostic Maze: Unraveling the Challenges of Diagnosis
Diagnosing bipolar disorder is often complex. There is no simple blood test or brain scan capable of definitively confirming the diagnosis. This makes the process of diagnosis a delicate balance of clinical observation, assessing the individual's history, and gathering information from their loved ones.
The symptoms of bipolar disorder can overlap with other mental health conditions, such as major depressive disorder, anxiety disorders, and even personality disorders. Moreover, the symptoms of these disorders can fluctuate, making them hard to pinpoint. Mania can sometimes be mistaken for simple elevated mood, while depression can be seen as a phase of sadness.
Accurate diagnosis, which hinges on an experienced clinician will assess the individual's presenting concerns, the family history of mental illness, and any past or ongoing substance use. It will involve a thorough evaluation of these symptoms. The individual's own self-report is crucial, providing an understanding of the internal experiences and the nature of the mood changes. However, it can also involve obtaining reports from the individual's family members. A history of manic or hypomanic episodes, and the characteristics of any depressive episodes. The frequency, severity, and duration of these episodes are crucial.
The need for continuous monitoring underscores the importance of ongoing care and support.
Treatment Strategies: Navigating the Path to Stability
The treatment of bipolar disorder is multifaceted, requiring a combination of medication, therapy, and lifestyle adjustments. There are many medications that can help regulate mood and stabilize the highs and lows.
Mood Stabilizers: These medications, such as lithium, are the cornerstone of bipolar disorder treatment, and help regulate mood swings by reducing the frequency and severity of episodes. The dosage must be carefully calibrated to avoid adverse effects.
Antipsychotics: These medications can be used to manage manic episodes and psychotic symptoms, such as hallucinations and delusions. They can also be used as a long-term mood stabilizer.
Antidepressants: Prescribed with caution, these medications can be used to treat depressive episodes, but care must be taken as they can sometimes trigger mania or hypomania.
Psychotherapy: Therapy is a crucial part of treatment, aiding individuals in developing coping strategies, managing symptoms, and understanding their illness. Cognitive behavioral therapy (CBT) can help identify and change negative thought patterns and behaviors, while interpersonal and social rhythm therapy (IPSRT) focuses on establishing and maintaining regular daily routines to stabilize mood.
Lifestyle Adjustments: Regular sleep, diet, and exercise are vital, and help regulate the body's natural rhythms and bolster overall mental health. Stress management techniques such as mindfulness and meditation can also prove beneficial.
The most crucial aspect of treatment is the collaboration between the individual, their healthcare providers, and their support network.
The Untold Stories: Lived Experiences and the Importance of Empathy
Beyond the clinical definitions and treatment plans, the experiences of individuals living with bipolar disorder are the essential aspect to understand. This condition impacts every facet of a person's life, from their relationships to their careers, and from their sense of self to their overall outlook.
The effects of manic episodes are often very detrimental to the affected individual's life. Employment and education can suffer. The reckless decisions, impulsivity, and impaired judgment can have serious repercussions. The individual might make impulsive job changes, quit school, or make poor investments. Relationships become strained, as the person's behavior becomes difficult to manage.
Depressive episodes carry their own set of challenges. Social withdrawal is common, as the individual loses interest in activities and struggles to engage with others. Employment can be affected, which can lead to financial and emotional difficulties. The individual may lose the drive to do the things they once loved.
The importance of empathy, understanding, and acceptance cannot be overstated. Those struggling with bipolar disorder need a supportive environment where they are not judged, stigmatized, or dismissed. They need to know that their experiences are validated, and that they are not alone.
Addressing Stigma: Breaking Down the Barriers
The stigma surrounding bipolar disorder is a significant barrier to seeking help and living a fulfilling life. Misconceptions and negative stereotypes often lead to shame, isolation, and discrimination.
People with bipolar disorder are often unfairly labeled as "crazy," "unstable," or "dangerous." Fear of being judged or rejected can prevent individuals from seeking professional help, opening up to friends and
